It’s a fair question, and a genuinely important one. Veneers are a significant investment, and if you’re considering them, you want to understand not just what they’ll do for the look of your smile — but whether they’ll affect the health of your gums and the long-term condition of your mouth.
The short answer is: well-placed veneers, in the right patient, are not bad for your gums. But placement quality matters enormously. Poorly designed veneers, veneers placed in the presence of active gum disease, or veneers that aren’t properly maintained can create conditions that harm gum tissue over time.
This post unpacks the evidence — what we know about how veneers interact with gum tissue, what the real risks are, and how to protect your gum health if you decide veneers are right for you. If you’re also wondering what to expect after placement, see our guide on veneers recovery time in Mindarie.
Quick Answer: Veneers are not inherently bad for your gums when they are properly designed, correctly placed by a qualified dentist, and maintained with good oral hygiene. Risks to gum health — such as mild irritation at the veneer margin or, in rare cases, gum recession — are primarily associated with poorly fitting veneers, inadequate margin placement, or neglected oral hygiene after treatment. Patients with active gum disease should have it treated before considering veneers.
Contents Navigation
- 1 How Do Veneers Interact with Your Gums?
- 2 Can Veneers Cause Gum Recession?
- 3 Gum Irritation After Veneers: What’s Normal and What Isn’t
- 4 What Makes a Veneer Safe for Gum Health?
- 5 How to Protect Your Gums with Veneers Long-Term
- 6 When Should You Be Concerned About Your Gums After Veneers?
- 7 Are Veneers Suitable If I Have Gum Disease?
- 8 About Veneers at Anchorage Dental Care, Mindarie
- 9 Frequently Asked Questions About Veneers and Gum Health
- 10 Book a Veneer Consultation at Anchorage Dental Care, Mindarie
How Do Veneers Interact with Your Gums?
A dental veneer is a thin shell — typically 0.3 to 0.7 millimetres thick — bonded to the front surface of a tooth. The edge of the veneer, called the margin, typically sits at or just below the gum line.
This relationship between the veneer margin and the gum tissue is where most gum-related concerns originate.
When the margin is well-designed and correctly placed:
- The transition between the veneer edge and tooth is smooth and flush
- Gum tissue can adapt comfortably around the veneer
- Plaque has no more foothold than it would around a natural tooth
- Normal brushing and flossing maintain gum health effectively
When the margin is poorly designed or incorrectly placed:
- A slight ledge or gap at the margin traps food debris and bacteria
- Plaque accumulates at the gum line, triggering inflammation
- Gum tissue becomes irritated, bleeds more easily, and may recede over time
- The veneer may also feel rough to the tongue, which is often the first sign of a margin issue
This is why the skill and care of the dentist placing your veneers matters as much as any other factor in their long-term success.
Can Veneers Cause Gum Recession?
Gum recession — where gum tissue gradually pulls back from the tooth, exposing more of the tooth root — is one of the concerns people raise about veneers.
Veneers themselves do not directly cause recession. The tooth root sits below the gum line; the veneer is on the front surface above it. A veneer, by itself, does not mechanically pull gum tissue downward.
However, certain veneer-related factors can contribute to recession risk:
- Margin placed too deep beneath the gum line. Placing the veneer margin too far subgingivally (below the gum line) can traumatise the biological width — the natural seal between your gum tissue and tooth surface. This is a known risk when excessive depth is pursued for purely aesthetic reasons (for example, to completely hide a preparation line). Properly trained dentists balance aesthetics with biological limits.
- Gum irritation leading to chronic inflammation. Ongoing gum inflammation from plaque accumulation at a poorly fitting margin is a risk factor for recession over time, just as active gum disease can cause recession around natural teeth.
- Overcontoured veneers. Veneers that are too thick, or that create a bulging profile, can put pressure on gum tissue or make it harder to clean effectively. Modern minimal-preparation porcelain veneers are designed specifically to avoid this.
- Underlying recession tendency. If a patient already has thin gum tissue or is prone to recession for genetic or lifestyle reasons (such as aggressive brushing), this tendency doesn’t disappear with veneers. It should be assessed and discussed before treatment.
The important qualification: Studies in dental literature generally show that well-designed porcelain veneers with supragingival margins (margins at or above the gum line) have minimal impact on gum tissue health, and gum health typically remains stable long-term in patients with good oral hygiene. The outcomes are significantly better when patients don’t have pre-existing gum disease.
Gum Irritation After Veneers: What’s Normal and What Isn’t
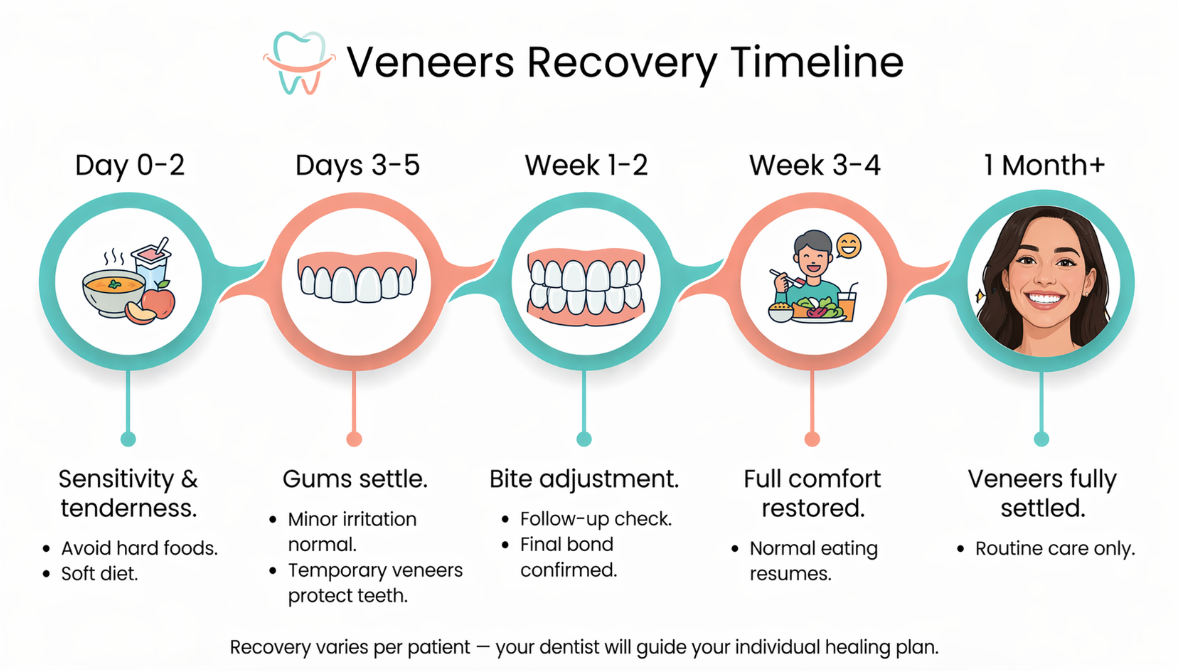
Some degree of gum response immediately after veneer placement is normal. Your gums have been worked around — temporarily separated, impressions taken, veneers fitted. They need a period to settle.
Normal in the first one to two weeks:
- Mild tenderness around the veneer edges, particularly when brushing
- Minor gum puffiness (edema) at the margins
- Light bleeding when flossing near the veneers
- General sensitivity in the gum tissue that improves progressively
Not normal — contact your dentist:
- Significant swelling that is getting worse, not better
- Persistent bright red gum tissue that doesn’t improve after two weeks of good hygiene
- Gum recession appearing in the weeks after placement
- White or ulcerated tissue near a veneer
- A veneer that consistently traps food and is difficult to clean despite good technique
- Persistent bleeding despite improved oral hygiene
If your gums haven’t settled within two to three weeks of placement, this warrants assessment. Early intervention on a minor fitting issue is far preferable to letting it develop into a more significant problem.
What Makes a Veneer Safe for Gum Health?
The factors that determine whether veneers are well-tolerated by your gum tissue:
1. The Margin Position
Margins placed at the gum line (supragingival) or just at the gum line (equigingival) are generally better tolerated than deeply subgingival margins. There are cosmetic situations where a slightly subgingival margin is appropriate, but this should be a deliberate, considered decision — not a default.
2. The Surface Finish
Porcelain has an inherently smooth, non-porous surface that plaque does not adhere to as readily as composite resin. High-quality porcelain veneers, properly polished, are among the most biocompatible dental materials available.
Composite veneers are slightly more porous and may accumulate stains and plaque over time if not maintained with careful polishing. This doesn’t make them harmful — it makes consistent hygiene maintenance more important.
3. The Fit
A veneer that fits precisely, with no overhanging edges, ledges, or gaps at the margin, gives bacteria nowhere to hide and gives your gum tissue the smoothest possible surface to seal against. Ill-fitting veneers are the primary source of gum problems.
4. The Design of the Prosthesis
Well-designed veneers maintain natural tooth contours — they don’t over-bulk the tooth profile. Overcontoured restorations are harder to clean and more likely to impinge on gum tissue.
5. Your Pre-Treatment Gum Health
This is non-negotiable: active gum disease must be treated before veneers are placed. Placing veneers in the presence of untreated periodontitis or active gingivitis will not resolve the underlying disease — it can actually make it harder to treat. Your dentist should assess and stabilise your gum health before any elective cosmetic work begins.
How to Protect Your Gums with Veneers Long-Term
Having veneers doesn’t change the fundamentals of gum health — it makes them more important, not less. The same habits that protect your natural teeth protect your veneers.
Brush Twice Daily — with Technique
Use a soft-bristled toothbrush and angle it at 45 degrees toward the gum line. The goal is to gently sweep plaque from the margin area, not to scrub hard at the tooth surface. Electric toothbrushes with pressure sensors are particularly helpful for patients who tend to brush aggressively.
Brushing too hard is one of the most common contributors to gum recession — not just around veneers, but around all teeth. If your toothbrush bristles are flattening within a few months, you’re likely brushing too hard.
Floss or Use Interdental Brushes Daily
The veneer margin runs along the sides of the tooth as well as the front. Plaque at the contacts between teeth — where the veneer meets adjacent teeth — needs to be removed mechanically. Flossing or using interdental brushes is not optional with veneers.
Water flossers are a useful addition, particularly for the margin area, but they don’t fully replace physical flossing.
Attend Regular Check-Ups and Cleans
Professional scaling removes calculus (hardened plaque) that home brushing can’t reach. Gum disease that begins to develop around veneers can be caught and reversed at an early stage with regular check-ups — but it won’t resolve itself without intervention.
At Anchorage Dental Care, we recommend regular six-monthly check-ups as the standard for veneer patients. Your dentist can also polish composite veneers during these visits to maintain their surface finish.
Don’t Grind or Clench
Bruxism (teeth grinding and clenching) places significant forces on veneers and can crack or chip them over time. It can also put abnormal forces on the gum tissue around the veneer margins. If you grind at night, a custom-fitted night guard should be part of your plan before or alongside veneer treatment.
Avoid Very Hard Foods
Chewing ice, biting fingernails, using your teeth as tools, or biting down on very hard foods directly applies force to the veneer bond. While modern porcelain veneers are remarkably durable, they are not indestructible.
When Should You Be Concerned About Your Gums After Veneers?
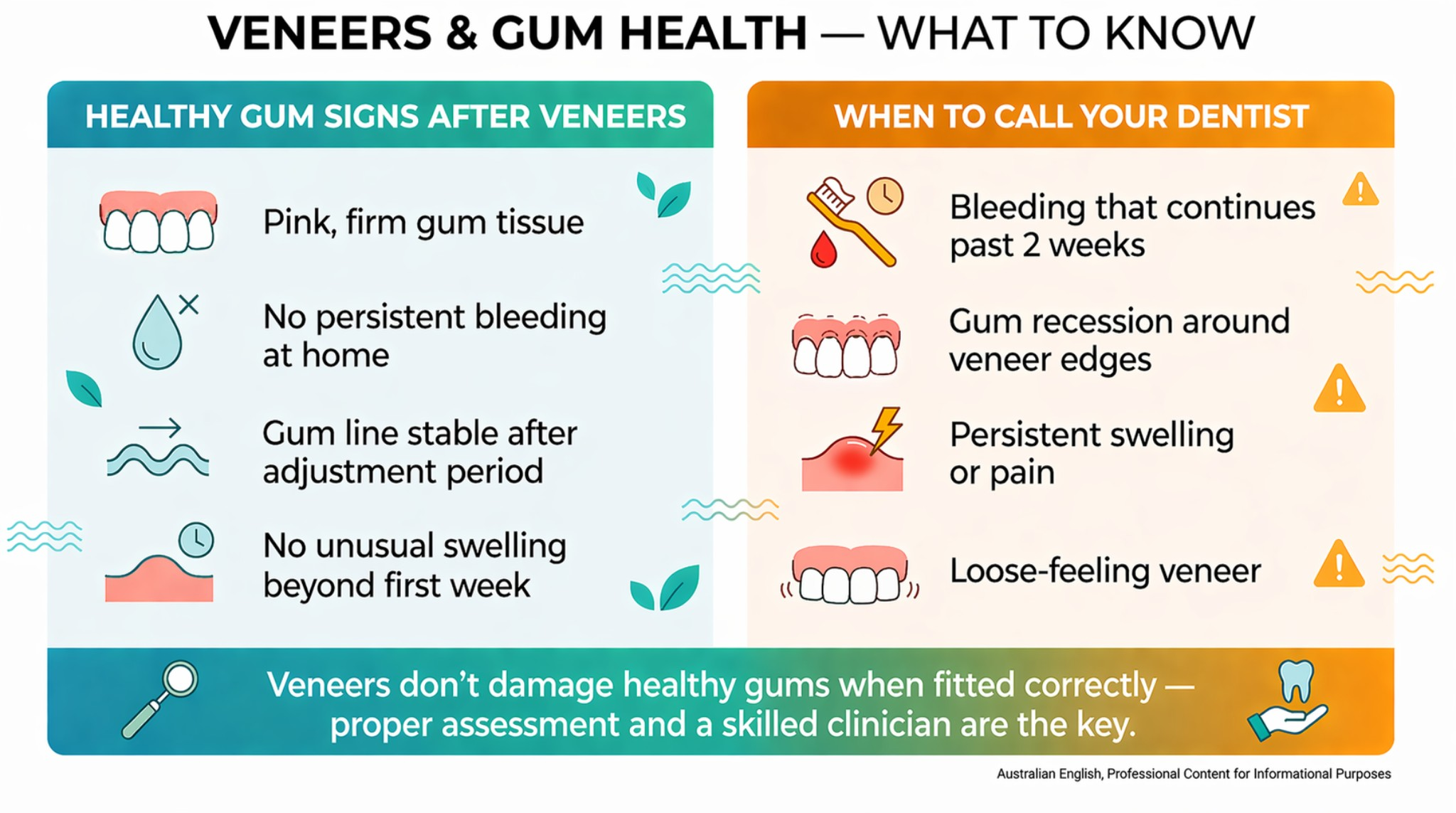
Watch for these signs and contact your dentist if they develop:
- Visible recession: You can see more of the tooth at the gum line than when the veneers were placed — the gum appears to be pulling back from the veneer edge
- Persistent redness or swelling around one or more veneers that doesn’t respond to improved hygiene
- Bleeding on brushing that continues beyond the first two weeks and doesn’t improve
- A veneer that feels rough or catches on dental floss — this is a margin issue
- Black triangles appearing between the veneer and adjacent tooth — this can indicate gum recession between teeth
- Looseness — a veneer that feels different to bite on, or that you can feel moving
Any of these warrants an appointment. Most early-stage issues are straightforward to address. Advanced issues take longer and are more complex to resolve.
Are Veneers Suitable If I Have Gum Disease?
No — not until the gum disease is treated and stable.
This is a firm clinical position, not a dental practice preference. Active periodontal disease means your gum tissue is in a state of inflammation and ongoing destruction. Placing cosmetic restorations over diseased gum tissue is not ethical, not in your long-term interest, and clinically unpredictable.
The sequence must be:
- Full periodontal assessment
- Non-surgical gum treatment (scale and clean, root planing if needed, oral hygiene instruction)
- Re-assessment — confirming gum disease is under control
- Continued monitoring to confirm stability (typically over several months)
- Then cosmetic consultation for veneers
Any dentist who proposes to place veneers over active gum disease without addressing the disease first should prompt you to seek a second opinion.
For more information on veneer suitability, see our post: Who Is Not Suitable for Veneers?
About Veneers at Anchorage Dental Care, Mindarie
At Anchorage Dental Care in Mindarie, our cosmetic consultations always include a thorough assessment of your gum health before any veneer treatment is discussed. We don’t believe in rushing to cosmetic outcomes before the foundations are sound.
We serve patients from Mindarie, Clarkson, Quinns Rocks, Merriwa, Alkimos, and the broader northern Perth coastal corridor. With 385+ Google reviews, we’ve helped many patients understand their cosmetic options clearly, including the questions most people are nervous to ask — like this one.
If you have questions about veneers, gum health, or whether veneers are right for your situation, a consultation is the best starting point. We’ll give you an honest assessment — including an honest answer if veneers aren’t the right choice for you right now.
Frequently Asked Questions About Veneers and Gum Health
Do veneers damage your gums?
Well-designed veneers placed by a qualified dentist, with correct margin position and proper fit, do not damage healthy gums. Gum problems associated with veneers are generally related to poor fit, margin placement issues, inadequate oral hygiene, or pre-existing gum disease — not the veneer material itself.
Can veneers cause gum recession?
Veneers themselves don’t directly cause recession, but factors related to their placement — particularly margins placed too deep below the gum line, chronic gum inflammation from plaque at a poorly fitting margin, or overcontoured veneers — can contribute to recession risk over time. Well-placed veneers with good home care have a low risk of causing recession.
How do I clean around my veneers to protect my gums?
Brush twice daily with a soft-bristled toothbrush angled toward the gum line, and floss or use interdental brushes daily. Avoid brushing aggressively. A water flosser can be a helpful addition for the margin areas. Regular professional cleans every six months help maintain the gum tissue around veneers long-term.
Can I get veneers if I have sensitive gums?
Gum sensitivity alone doesn’t necessarily disqualify you from veneers, but the cause needs to be assessed first. If sensitivity is related to gum recession, thin gum tissue, or active gum inflammation, these factors need to be addressed and stabilised before cosmetic treatment proceeds.
What happens to the gums under a veneer over time?
In patients with healthy gums and well-placed veneers, gum tissue typically remains stable over time. Studies generally show that high-quality porcelain veneers have minimal long-term impact on gum health in appropriately selected patients who maintain good oral hygiene.
Should I tell my dentist about a family history of gum disease before getting veneers?
Yes — this is relevant information. A family history of periodontitis can increase your risk. Your dentist should complete a full periodontal assessment before any veneer treatment, including probing depths and gum health indicators, to confirm your gum tissue is healthy and stable enough for cosmetic work.
Book a Veneer Consultation at Anchorage Dental Care, Mindarie
If you’ve been weighing up veneers but have concerns about your gum health, the answer starts with a proper clinical assessment — not guesswork from an online article.
Our team will examine your gums, your teeth, and your overall oral health, and give you an honest picture of whether veneers are appropriate for you and what the process would involve. No pressure, no rush.
📞 Call us to book your consultation, or visit anchoragedental.com.au to book online.
Anchorage Dental Care — Building Brighter Smiles with Your Dentist in Mindarie.
Sources and References
- Australian Dental Association (ADA) — dental.org.au
- AHPRA dental advertising guidelines — ahpra.gov.au
- Healthdirect Australia — healthdirect.gov.au
- Journal of Prosthetic Dentistry (peer-reviewed dental literature)
- Australian Dental Journal (peer-reviewed dental literature)
Published: April 2026. Reviewed by: Anchorage Dental Care Clinical Team.
Related post: Who Is Not Suitable for Veneers?